The New Rules Of Mental Health Care, Where Science, Style, And Self-Awareness Meet
There was a time when mental health care lived on the margins of public conversation, tucked behind closed doors and softened with euphemisms. That era is over. Today, therapy appointments sit on calendars next to Pilates classes and board meetings. Conversations about burnout unfold at dinner parties without a drop in volume. The language has changed, but more importantly, the expectations have changed. People want care that fits their lives, their values, and their sense of identity.
Modern treatment is no longer framed as a last resort. It is a proactive choice, one that reflects self-respect rather than crisis. Clinicians are responding in kind. Programs now blend evidence-based therapy with lifestyle support, from nutrition guidance to sleep stabilization to structured digital detox plans. It feels less like entering a sterile system and more like stepping into a comprehensive health strategy. That shift has made it easier for people to seek support early, rather than waiting until they are overwhelmed.
Access Expands Beyond Geography
For years, location dictated options. If you lived in a major city, you likely had access to specialists. If you did not, your choices narrowed quickly. That divide is shrinking. Telehealth platforms have widened the field, allowing people to connect with licensed clinicians across state lines, attend group therapy online, and even participate in structured outpatient programs from home.
At the same time, in-person care is evolving in major metropolitan hubs. From boutique outpatient clinics to hospital-affiliated programs, mental health services in Los Angeles, New York or anywhere in between are expanding in both scope and design. Waiting rooms look less clinical and more considered. Treatment plans are personalized rather than standardized. The message is clear, care should not feel like an afterthought. It should feel integrated into the fabric of daily life.
Insurance coverage has also broadened, albeit unevenly. More employers are adding comprehensive mental health benefits to their packages, recognizing that productivity and wellbeing are intertwined. That corporate acknowledgment, once rare, has become a marker of progressive workplace culture.
Beyond Talk Therapy, The Rise Of Integrated Treatment
Traditional psychotherapy remains a cornerstone, and for good reason. Cognitive behavioral therapy, dialectical behavior therapy, and trauma-informed approaches continue to show strong outcomes. Yet clinicians increasingly pair these methods with complementary strategies that address the body as well as the mind.
Medication management has become more precise, with psychiatrists tailoring dosages carefully and monitoring side effects with greater transparency. At the same time, lifestyle interventions are no longer relegated to footnotes. Sleep hygiene is treated as foundational. Movement is framed as medicine, not punishment. Nutritional psychiatry is gaining traction, examining how gut health and micronutrients influence mood and cognition.
Some programs incorporate mindfulness training and breathwork, not as trends but as tools that can help regulate the nervous system. Others weave in creative therapies such as art or music to support emotional processing. The result is a treatment model that feels multidimensional. It recognizes that people are not collections of symptoms but whole, complex individuals navigating layered lives.
Community, Identity, And The Power Of Group Work
Individual therapy offers depth and privacy, yet many people discover that healing accelerates in community. Group therapy has shed outdated stereotypes and emerged as a powerful setting for connection. Participants often describe relief in hearing someone articulate a thought they assumed was uniquely theirs. That shared recognition can loosen isolation in a way that one-on-one work sometimes cannot.
Programs are increasingly tailored to specific populations, whether that means young adults navigating early career stress, parents balancing caregiving and ambition, or older adults facing transitions in health and identity. Cultural competence has become a priority, with clinicians receiving training to understand how race, gender, sexuality, and socioeconomic background shape mental health experiences.
This attention to identity matters. When people feel seen in the full context of their lives, treatment tends to resonate more deeply. It moves beyond symptom management and toward sustainable change, grounded in real-world circumstances rather than abstract ideals.
Technology Enters The Therapy Room
Digital tools are no longer an accessory to treatment, they are part of its architecture. Mood tracking apps allow patients and clinicians to spot patterns between sessions. Secure messaging platforms create continuity. Virtual reality exposure therapy is being used to help individuals face specific fears in controlled settings. Wearable devices can monitor sleep and heart rate variability, offering data that informs care plans.
The conversation around AI and mental healthcare has grown louder, and with good reason. Artificial intelligence is being used to analyze speech patterns for signs of mood shifts, to flag risk factors in electronic health records, and to power chat-based support tools that offer immediate coping strategies. While these technologies are not replacements for human clinicians, they can extend reach and improve responsiveness. Used thoughtfully, they support rather than supplant the therapeutic relationship.
Ethical oversight remains essential. Privacy protections, informed consent, and algorithm transparency are active topics of discussion. Still, the potential is significant. Technology can reduce barriers, particularly for those who feel intimidated by traditional settings or who live far from specialized providers.
Prevention As The New Priority
One of the most encouraging developments is the growing emphasis on prevention. Schools are integrating social and emotional learning into curricula. Workplaces are offering resilience workshops and stress management training before burnout spirals. Primary care physicians are screening for depression and anxiety during routine visits, treating mental health as inseparable from physical health.
This proactive stance reframes the narrative. Care is not about fixing what is broken. It is about maintaining balance and building skills that support long-term wellbeing. The earlier people engage with tools such as cognitive reframing, emotional regulation, and boundary setting, the more resilient they tend to feel when life inevitably becomes complicated.
A Future That Feels Personal
Mental health care is moving toward a model that feels both high-tech and deeply human. It honors science while acknowledging that healing is rarely linear. It respects individuality without abandoning evidence. Most of all, it invites participation rather than silence.
There is still work to do. Access gaps persist, stigma lingers in certain communities, and insurance complexities can frustrate even the most determined patient. Yet the direction is promising. Treatment today looks less like a last resort and more like an informed choice woven into modern life.
Mental health care no longer sits in the background of cultural conversation. It has stepped into the foreground, reshaped by innovation, empathy, and a collective willingness to speak plainly about what it means to struggle and to recover. As treatment options continue to expand and adapt, the opportunity is not simply to manage distress but to build a life that feels aligned and supported. That is not indulgence. It is intelligent, intentional care, and it is becoming the new standard.
POSTS ACROSS THE NETWORK

The Technology Reshaping UK Medical Cannabis Services

The Compounding Problem in Agentic AI Era
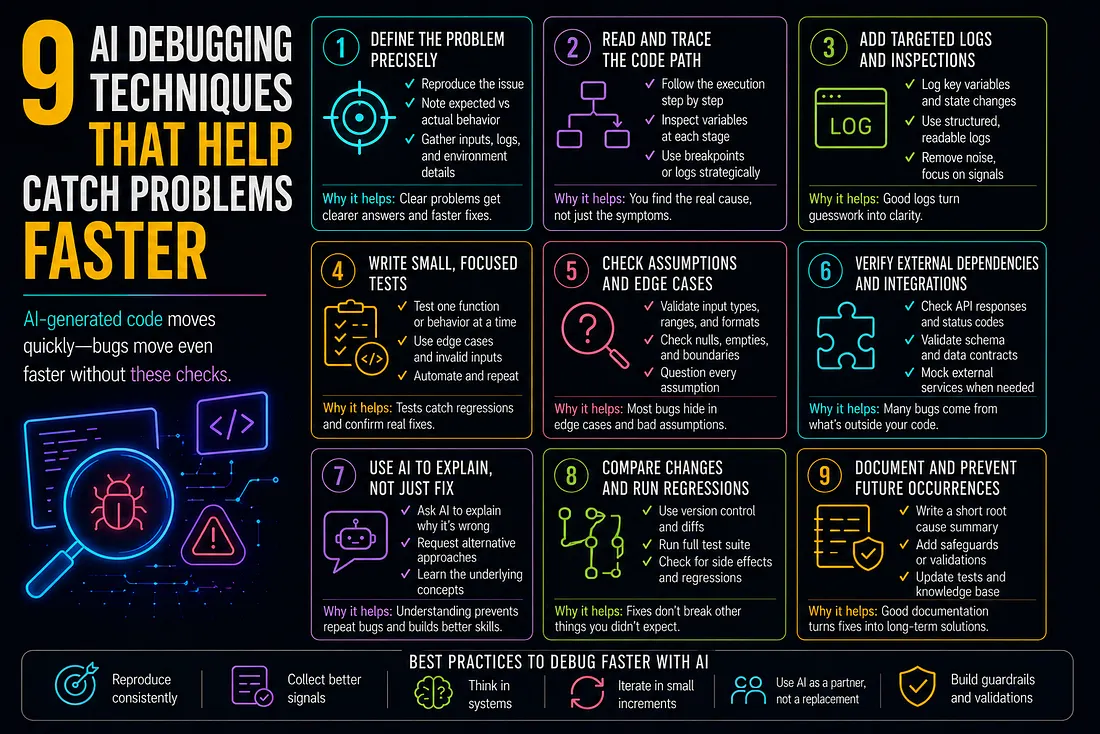
9 AI Debugging Techniques That Help Catch Problems Faster
How to Add SMS to Marketo Smart Campaigns Without Breaking Your Workflow
Best MCP Server for SEO in 2026: Guide for GEO, AEO, and SERM Experts